Calcium Metabolism | Vibepedia
Calcium metabolism encompasses the complex processes governing the absorption, distribution, and excretion of calcium within the body, with bone serving as a…
Contents
Overview
The understanding of calcium metabolism has evolved over centuries, with early observations dating back to ancient physicians recognizing the importance of bone. However, the scientific unraveling of its hormonal regulation began in the early 20th century. Key breakthroughs included the identification of the parathyroid glands and their role in calcium balance, a field significantly advanced by endocrinologists like Fuller Albright. His meticulous clinical observations and experimental work at Massachusetts General Hospital in the mid-20th century illuminated conditions like hyperparathyroidism and hypoparathyroidism, establishing the direct link between these glands and calcium homeostasis. The discovery and characterization of Vitamin D's role as a crucial mediator for intestinal calcium absorption, largely by researchers like Hector DeLuca, further cemented the complex interplay of hormones and nutrients governing calcium levels.
⚙️ How It Works
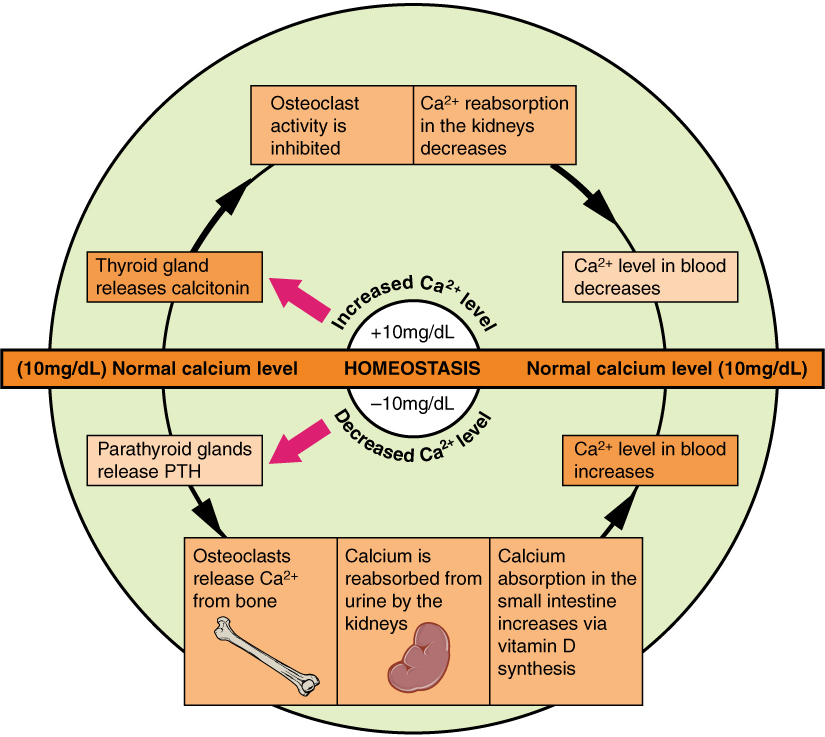
At its core, calcium metabolism is a dynamic system involving absorption in the gastrointestinal tract, distribution via the bloodstream, deposition and withdrawal from bone, and excretion through the kidneys and feces. The intestinal absorption of calcium is largely dependent on Vitamin D and is an active process requiring specific transport proteins. Once in the plasma, calcium exists in several forms: protein-bound, complexed with anions, and ionized. The ionized fraction is biologically active and tightly regulated. Bone remodeling, a continuous process of bone resorption by osteoclasts and formation by osteoblasts, allows the skeleton to act as a vast calcium bank, releasing calcium into the blood when needed and sequestering excess calcium. The kidneys play a vital role in filtering calcium and reabsorbing it, a process influenced by PTH, thereby controlling urinary calcium excretion.
📊 Key Facts & Numbers
The human body typically contains about 1 to 1.5 kg of calcium, with over 99% stored in the skeleton. Plasma calcium levels are maintained within a remarkably narrow range, typically 8.5 to 10.2 mg/dL (2.1 to 2.55 mmol/L). Over 50% of plasma calcium is ionized, the biologically active form. Approximately 40% is bound to plasma proteins, primarily albumin. The recommended daily intake of calcium varies by age and physiological state, with adults generally advised to consume between 1000 to 1300 mg per day. Insufficient calcium intake or absorption can lead to a significant increase in the prevalence of osteoporosis, affecting an estimated 200 million people worldwide. Kidney stones, often composed of calcium oxalate, are a common manifestation of calcium dysregulation, affecting up to 10% of the population at some point in their lives.
👥 Key People & Organizations
Pioneering endocrinologists like Fuller Albright (1897-1969), an American physician and researcher, made seminal contributions to understanding calcium and bone disorders. His work at Massachusetts General Hospital defined many classic endocrine syndromes related to calcium. Hector DeLuca (1930-2017), a biochemist at the University of Wisconsin–Madison, was instrumental in elucidating the metabolism and function of Vitamin D, earning him the nickname "the father of Vitamin D." Key organizations like the National Osteoporosis Foundation and the Endocrine Society are at the forefront of research, education, and advocacy concerning calcium metabolism and bone health. Pharmaceutical companies such as Amgen and Novartis are major players in developing treatments for calcium-related disorders.
🌍 Cultural Impact & Influence
Calcium's role extends far beyond bone health, permeating cellular physiology and influencing broader cultural perceptions of health and wellness. The understanding of calcium's signaling role in muscle contraction and neurotransmitter release has profoundly impacted fields from neuroscience to sports medicine. Public health campaigns promoting dairy consumption and calcium supplementation, often spearheaded by organizations like the Dairy Council, have shaped dietary guidelines and food product development for decades. The aesthetic ideal of strong, healthy bones and teeth, often associated with youth and vitality, is deeply ingrained in popular culture, influencing everything from advertising to beauty standards. Conversely, the association of calcium with kidney stones has also contributed to a more cautious public perception, leading some to actively limit intake.
⚡ Current State & Latest Developments
Current research is intensely focused on the gut microbiome's influence on calcium absorption and bone health, with studies exploring how specific bacterial species might modulate nutrient uptake and inflammatory pathways. Advances in genetic sequencing are identifying novel genes and mutations that predispose individuals to rare calcium disorders, paving the way for targeted therapies. The development of biologics, such as denosumab (Prolia), represents a significant leap in managing bone loss by targeting the RANKL pathway, which is crucial for osteoclast activity. Furthermore, there's growing interest in the role of calcium signaling in chronic diseases beyond bone, including cardiovascular disease and certain cancers, with ongoing investigations into therapeutic interventions that modulate calcium flux.
🤔 Controversies & Debates
A persistent debate revolves around optimal calcium intake, particularly the balance between preventing osteoporosis and the potential increased risk of kidney stones and cardiovascular events, especially with high-dose supplementation. While the FDA generally recommends adequate calcium intake, some meta-analyses have suggested a link between high calcium supplement use and increased risk of cardiovascular events, though this remains a contentious area with conflicting evidence. The role of dietary versus supplemental calcium is also debated, with some researchers arguing that dietary sources are safer and more effective due to the presence of other synergistic nutrients. The precise mechanisms by which calcium supplements might influence cardiovascular health, including potential effects on vascular calcification, are still under active investigation and subject to considerable scientific disagreement.
🔮 Future Outlook & Predictions
The future of calcium metabolism research likely lies in personalized medicine, leveraging genetic profiling to tailor calcium and Vitamin D recommendations to individual needs and predispositions. We can expect to see the development of novel therapeutic agents that more precisely target calcium regulatory pathways, potentially offering solutions for conditions currently resistant to treatment. The exploration of the gut-bone axis will undoubtedly yield new insights, leading to probiotic or prebiotic interventions aimed at improving calcium homeostasis. Furthermore, advancements in imaging techniques may allow for more accurate assessment of bone microarchitecture and calcium deposition in soft tissues, enabling earlier and more precise diagnosis of metabolic bone diseases and vascular calcification.
💡 Practical Applications
Calcium metabolism has direct and profound practical applications across medicine and nutrition. In clinical practice, understanding calcium levels is crucial for diagnosing and managing a wide array of endocrine and metabolic disorders, including hyperparathyroidism, hypoparathyroidism, osteoporosis, rickets, and osteomalacia. Nutritional science relies heavily on calcium metabolism principles to formulate dietary guidelines and fortification strategies for foods like milk, cereals, and juices, aiming to prevent deficiencies. In sports medicine, adequate calcium intake is vital for athletes to maintain bone density and prevent stress fractures. The pharmaceutical industry develops drugs that modulate calcium absorption, excretion, or bon
Key Facts
- Category
- science
- Type
- topic